Living with diabetes well means understanding that it’s a marathon, not a sprint. The good news is, by making consistent, practical changes to your daily routine, you can significantly improve your quality of life. It’s about finding a rhythm that works for you, not following a rigid, one-size-fits-all plan. This isn’t about perfection; it’s about progress and consistently making choices that support your health.
Before diving into lifestyle changes, it’s really helpful to get a solid grasp on what type of diabetes you have and how it affects your body. There’s a difference between Type 1, Type 2, and gestational diabetes, and they each come with their own nuances.
Type 1 vs. Type 2: Know the Difference
Type 1 diabetes is an autoimmune condition where your body doesn’t produce insulin. It’s not caused by lifestyle choices. Type 2 diabetes, on the other hand, is much more common and often develops over time, either because your body doesn’t produce enough insulin or doesn’t use it effectively (insulin resistance). Gestational diabetes occurs during pregnancy and usually resolves after birth, but it can increase the risk of developing Type 2 later. Knowing which one applies to you is foundational because it guides your treatment plan.
The Role of Your Healthcare Team
You’re not in this alone. Your doctor, a certified diabetes educator (CDE), and a registered dietitian (RD) are your allies. They can help you understand your blood sugar targets, medication (if needed), and how food and activity impact your body. Don’t hesitate to ask questions – that’s what they’re there for. Building a good relationship with this team is a crucial step in managing your diabetes effectively. They can tailor advice to your specific needs and track your progress over time.
For those interested in exploring how lifestyle changes can impact health, particularly for managing diabetes, a related article that offers practical insights is available at Cultivate an Urban Homestead: Practical Ideas to Try. This article discusses various sustainable practices that can enhance your well-being and potentially aid in diabetes management through improved nutrition and physical activity.
Fueling Your Body: Smart Eating Strategies
What you eat plays a huge role in managing blood sugar. This isn’t about strict deprivation, but rather making informed choices that can help stabilize glucose levels and provide sustained energy. It’s about building sustainable habits, not just short-term fixes.
Carbohydrates: Quantity and Quality Matter
Carbohydrates have the biggest impact on blood sugar. This doesn’t mean you have to avoid them entirely; it means being mindful of how much you’re consuming and choosing complex, fiber-rich options over refined ones.
Understanding Net Carbs and Glycemic Index
Net carbs are total carbs minus fiber. Fiber doesn’t raise blood sugar, so focusing on net carbs can be helpful. The glycemic index (GI) ranks foods based on how quickly they raise blood sugar. Opting for low-GI foods, like whole grains, legumes, and most vegetables, can help prevent spikes. Foods like white bread, sugary drinks, and highly processed snacks tend to have a high GI.
Portion Control for Stable Blood Sugar
Even healthy carbs need to be consumed in appropriate portions. Using measuring cups, a food scale, or even just your hand as a guide can help keep things in check. A CDE or RD can help you determine the right carb intake for your individual needs and activity level. Think about spreading your carb intake throughout the day rather than eating large amounts in one go.
Protein and Healthy Fats: Your Blood Sugar Allies
Protein and healthy fats don’t significantly impact blood sugar directly, but they play crucial roles. They help you feel full and satisfied, which can prevent overeating, and they can slow down the absorption of carbohydrates, leading to a more gradual rise in blood sugar.
Lean Protein Sources
Include lean proteins like chicken, fish, tofu, beans, and lentils in your meals. Aim for a source of protein at each meal and snack. This helps with satiety and muscle maintenance. Adequate protein intake is also important for various bodily functions and can help prevent muscle loss, which is important for metabolism.
Incorporating Healthy Fats
Focus on unsaturated fats found in avocados, nuts, seeds, and olive oil. These fats are good for heart health, which is particularly important for people with diabetes, as they have a higher risk of heart disease. Limit saturated and trans fats found in processed foods and some animal products.
Fiber: The Unsung Hero
Fiber is incredibly beneficial for diabetes management. It slows down sugar absorption, helps with satiety, and supports gut health. Aim for at least 25-30 grams of fiber per day.
Boosting Fiber Intake Naturally
Load up on vegetables, fruits (with the skin on), whole grains, legumes, and nuts. Adding a handful of berries to your oatmeal or a side of steamed broccoli to your dinner are easy ways to increase your fiber. Fiber also helps regulate bowel movements, which contributes to overall digestive health.
Moving Your Body: The Power of Physical Activity

Regular physical activity is one of the most effective tools for managing diabetes. It helps your body use insulin more efficiently, lowers blood sugar, and contributes to overall well-being. The key is to find activities you enjoy and can stick with.
Finding Your Movement Groove
You don’t need to become a marathon runner overnight. Even small bursts of activity can make a difference. The goal is to move more and sit less.
Aerobic Exercise: Heart Health and Blood Sugar Control
Aim for at least 150 minutes of moderate-intensity aerobic activity per week, spread throughout the week. This could be brisk walking, swimming, cycling, dancing, or hiking. These activities get your heart rate up and improve insulin sensitivity. Think about activities that you genuinely enjoy, as this significantly increases the likelihood that you’ll keep doing them.
Strength Training: Building Muscle for Better Metabolism
Incorporate strength training exercises at least two times a week. This could involve lifting weights, using resistance bands, or bodyweight exercises like squats and push-ups. Muscle tissue uses more glucose than fat tissue, so building muscle helps improve insulin sensitivity and glucose uptake.
Managing Activity Safely
Before starting any new exercise routine, especially if you’re new to it or have complications, talk to your doctor. They can help you determine what’s safe and appropriate for you.
Monitoring Blood Sugar Before and After Exercise
Exercise can lower blood sugar, so it’s important to monitor your levels, especially when you’re starting out or trying a new activity. You might need to adjust your medication or snack intake. Always carry a fast-acting carb source (like glucose tablets or juice) in case of hypoglycemia. Understanding how your body reacts to different types of exercise will help you plan accordingly.
Staying Hydrated
Drink plenty of water before, during, and after exercise. Dehydration can affect blood sugar levels and overall performance. Water is essential for every bodily function, and it’s even more crucial when you’re active.
Continuous Monitoring and Medication Management
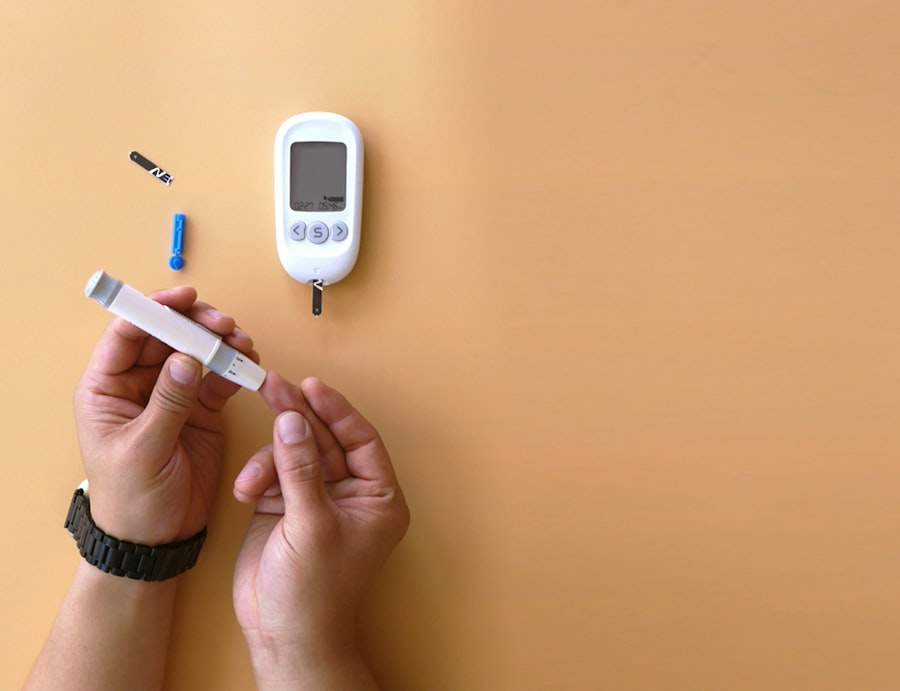
Keeping track of your blood sugar levels provides invaluable data that helps you and your healthcare team make informed decisions. For many, medication is also a critical component of diabetes management.
The Importance of Regular Blood Sugar Checks
Whether you use a traditional blood glucose meter or a continuous glucose monitor (CGM), consistent monitoring helps you understand how different foods, activities, and stress levels affect your blood sugar.
Understanding Your Target Ranges
Your doctor will set personalized target ranges for your blood sugar. Knowing these numbers helps you determine if your current lifestyle choices and medication are working effectively. Don’t compare your numbers to others; focus on your individualized goals.
Interpreting Your Data
Look for patterns. Are your blood sugars consistently high after certain meals? Do they drop too low after a particular exercise? This information is gold and can help you and your medical team fine-tune your management plan. Keep a log, either paper or digital, to notice these trends more easily.
Medication Adherence (If Applicable)
If your doctor has prescribed medication, whether it’s insulin, oral medications, or other injectables, taking them as directed is crucial for managing your blood sugar effectively.
Understanding Your Medications
Know the name of your medication, how it works, the correct dosage, and when to take it. Don’t hesitate to ask your pharmacist or doctor if anything is unclear. Understanding why you’re taking a particular medication can increase your adherence.
Addressing Side Effects and Concerns
If you experience side effects or have concerns about your medication, communicate them with your doctor immediately. Never adjust your dosage or stop taking medication without consulting your healthcare provider. There might be alternatives or strategies to mitigate side effects.
For those interested in managing diabetes through natural methods, exploring organic gardening techniques can be beneficial. Engaging in gardening not only promotes physical activity but also allows individuals to grow their own fresh produce, which can be a healthier alternative to processed foods. If you’re curious about how to cultivate your own garden while reaping the health benefits, you can read more in this informative article on organic gardening techniques. This approach can complement a diabetes management plan by providing access to nutritious fruits and vegetables.
Prioritizing Mental Well-being and Stress Reduction
“`html
| Metrics | Value |
|---|---|
| Prevalence of diabetes | 9.3% of the US population |
| Diabetes-related deaths | 1.5 million deaths per year |
| Diabetes type 1 vs type 2 | 5-10% have type 1, 90-95% have type 2 |
| Diabetes-related healthcare costs | 327 billion per year in the US |
“`
Living with a chronic condition like diabetes can be challenging, and it’s easy to overlook the impact of stress and emotional health on your physical well-being. These factors can directly affect blood sugar levels.
Recognizing the Link Between Stress and Blood Sugar
When you’re stressed, your body releases hormones like cortisol and adrenaline. These hormones are designed to give you a burst of energy in a perceived threat, but they also raise blood sugar by making the liver produce more glucose and making cells more resistant to insulin.
Identifying Your Stress Triggers
Take some time to notice what situations or thoughts tend to make you feel stressed. Is it work pressure, family dynamics, financial worries, or simply the daily grind of managing diabetes itself? Becoming aware of these triggers is the first step in addressing them.
Developing Healthy Coping Mechanisms
Instead of reaching for unhealthy comfort foods, try to find positive ways to cope. This could be anything from a short walk, listening to music, deep breathing exercises, spending time in nature, or connecting with friends and family. Experiment to find what genuinely helps you unwind.
Making Space for Self-Care
Self-care isn’t selfish; it’s essential for sustainable diabetes management. It means consciously taking steps to nurture your emotional, mental, and physical health.
Prioritizing Sleep Quality
Poor sleep can impact insulin sensitivity and make blood sugar harder to control. Aim for 7-9 hours of quality sleep each night. Establish a consistent sleep schedule, create a relaxing bedtime routine, and make sure your sleep environment is conducive to rest. Avoid screens an hour before bed and limit caffeine and heavy meals late in the evening.
Seeking Support When Needed
Don’t be afraid to reach out. Talk to trusted friends or family members, join a diabetes support group, or consider therapy if you’re struggling with anxiety, depression, or burnout related to your condition. A mental health professional can provide strategies for coping and managing the emotional load. Sharing your experiences can also be incredibly validating and help you realize you’re not alone.
By consistently applying these practical strategies, you’re not just managing a condition; you’re actively building a healthier, more fulfilling life for yourself. It’s a continuous learning process, so be patient, be kind to yourself, and celebrate every small victory along the way.


