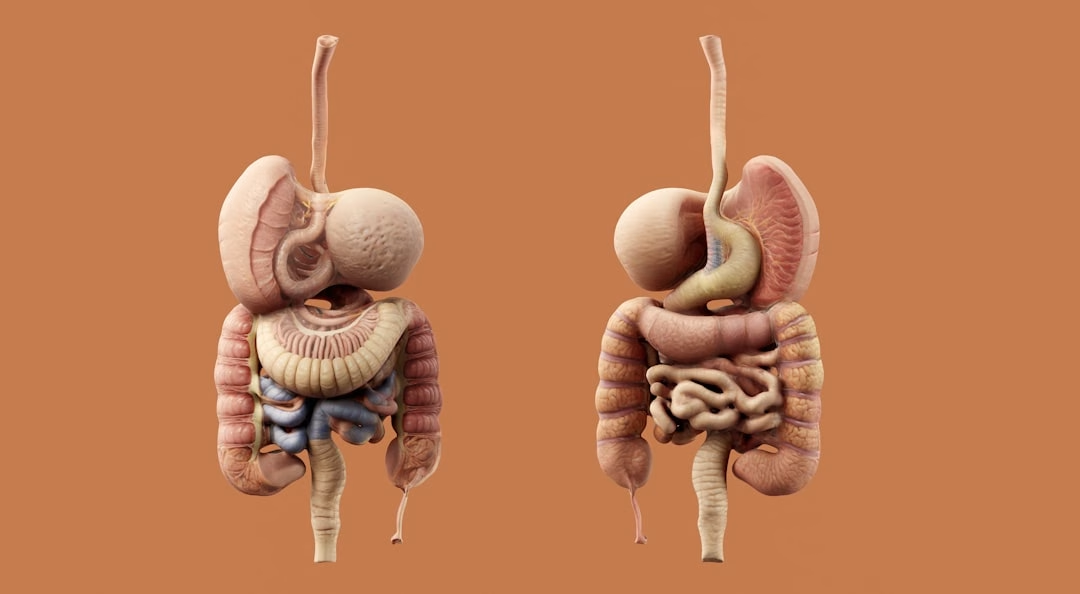
Ever had that gnawing, burning pain in your stomach, especially when it’s empty? That could be a stomach ulcer, also known as a gastric ulcer. Essentially, it’s an open sore that develops on the lining of your stomach, and sometimes on the first part of your small intestine (duodenum), which is then called a duodenal ulcer. The most common culprits? A bacterial infection called H. pylori and prolonged use of certain pain relievers. While they can be pretty uncomfortable, even painful, the good news is that they’re usually treatable.
To get a clearer picture, think of your stomach lining. It’s normally quite robust, designed to withstand the strong acids it uses for digestion. However, sometimes this protective layer gets damaged, allowing stomach acid to erode the tissue, leading to an open sore. This isn’t just a surface scratch; it can actually go quite deep.
Gastric vs. Duodenal Ulcers
While both are types of peptic ulcers, they appear in different locations and can sometimes present with slightly different symptoms:
- Gastric Ulcers: These are specifically in the stomach lining. The pain from these often gets worse shortly after eating, as food stimulates acid production.
- Duodenal Ulcers: These are found in the first part of the small intestine, right after the stomach. Pain from duodenal ulcers often improves with food but returns a few hours later when the stomach empties and acid levels rise. This is why people with duodenal ulcers might experience pain during the night.
Stomach ulcers, also known as peptic ulcers, can be a painful and disruptive condition, but there are various natural remedies that may help alleviate symptoms and promote healing. For those interested in exploring holistic approaches to health, a related article can be found at Explore Natural Remedies for a Healthier Life, which discusses various natural treatments that may support digestive health and overall well-being.
The Usual Suspects: Causes of Ulcers
It’s a common misconception that stress or spicy food directly cause ulcers. While these can certainly aggravate symptoms, they aren’t the primary cause. The vast majority of ulcers stem from just a couple of main issues.
Helicobacter pylori (H. pylori) Infection
This is the sneaky bacteria responsible for a large percentage of stomach and duodenal ulcers. It’s quite common, and many people carry it without ever developing an ulcer. However, in some individuals, it can:
- Inflame the Stomach Lining: H. pylori can weaken the protective mucus layer in your stomach.
- Increase Acid Production: The bacteria can also trigger your stomach to produce more acid.
- Direct Damage: In some cases, the bacteria can directly damage the cells lining the stomach or duodenum.
How do you get H. pylori? It’s thought to spread through contaminated food or water, or direct contact with an infected person’s saliva. Many people acquire it in childhood.
Long-Term Use of NSAIDs
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) are a broad class of pain relievers, and they’re incredibly common. Think ibuprofen (Advil, Motrin), naproxen (Aleve), and even aspirin. While they’re great for reducing pain and inflammation, they come with a potential downside for your stomach lining.
- How NSAIDs Cause Damage: NSAIDs work by blocking certain enzymes (cyclooxygenases or COX enzymes) that produce prostaglandins. Prostaglandins are natural chemicals in your body that, among other things, help protect your stomach lining by promoting mucus production and reducing acid. When NSAIDs block these, the stomach’s defenses are weakened, making it vulnerable to acid.
- Risk Factors with NSAIDs: The risk of developing an ulcer from NSAIDs increases with higher doses, longer duration of use, being over 60, having a history of ulcers, and taking other medications like corticosteroids or anticoagulants.
Less Common Causes
While H. pylori and NSAIDs account for most ulcers, there are a few other, less frequent culprits:
- Zollinger-Ellison Syndrome: This is a rare condition where tumors (gastrinomas) in the pancreas or duodenum produce excessive amounts of gastrin, a hormone that stimulates stomach acid production. The result is severe, multiple, and often difficult-to-treat ulcers.
- Other Medications: Certain medications, though far less common than NSAIDs, can increase ulcer risk, such as some chemotherapy drugs or bisphosphonates (used for osteoporosis).
- Serious Illness or Injury: In very severe cases, extreme physiological stress on the body (like major burns, head trauma, or critical illness) can lead to “stress ulcers.” These are more superficial and usually occur during the acute phase of the illness.
- Alcohol and Smoking: While not direct causes, heavy alcohol consumption and smoking can hinder the healing of ulcers and increase the risk of developing them, especially in combination with H. pylori or NSAID use. They both irritate the stomach lining and reduce its protective mechanisms.
What Does an Ulcer Feel Like? Signs and Symptoms

The most common symptom is that familiar burning stomach pain. But ulcers can present in a few different ways, and sometimes, they don’t cause any symptoms at all until complications arise.
Common Symptoms
- Burning Stomach Pain: This is the hallmark. It’s often described as a gnawing, aching, or searing pain. It typically occurs between meals or during the night when the stomach is empty.
- Indigestion/Heartburn: A feeling of fullness, bloating, or burning in the upper abdomen.
- Nausea and Vomiting: Especially after meals, or in more severe cases, vomiting blood.
- Tenderness to Touch: Your abdomen might feel tender when pressed.
Less Common but Serious Symptoms (Complications)
These indicate an ulcer might be getting worse or causing a serious issue and warrant immediate medical attention.
- Dark or Black Stools (Melena): This indicates bleeding in the upper digestive tract. The blood has been digested, turning the stool tar-like.
- Vomiting Blood (Hematemesis): This can appear bright red or look like “coffee grounds” if the blood has been in the stomach for a while.
- Unexplained Weight Loss: Can be a sign of a more serious underlying issue or chronic blood loss.
- Severe, Sharp Abdominal Pain: Could indicate a perforation, where the ulcer has eaten completely through the stomach or intestinal wall, a medical emergency.
- Anemia (Fatigue, Weakness, Paleness): Chronic, slow bleeding from an ulcer can lead to iron deficiency anemia over time.
Getting a Diagnosis: What to Expect
If you suspect an ulcer, it’s important to see a doctor. Self-diagnosing and self-treating can delay proper care and lead to complications.
Medical History & Physical Exam
Your doctor will ask about your symptoms, lifestyle, medication use (especially NSAIDs), and family history. They’ll also perform a physical exam, which usually involves feeling your abdomen.
H. pylori Tests
Since this bacterium is a major cause, your doctor will likely test for it. Several methods exist:
- Urea Breath Test: You drink a special liquid, and if H. pylori is present, it breaks down the liquid, releasing a gas that’s detected in your breath.
- Stool Antigen Test: This checks for H. pylori proteins in your stool.
- Blood Test: This checks for antibodies to H. pylori. However, a positive blood test means you’ve been exposed, but doesn’t necessarily mean you have an active infection. It’s less useful for confirming current infection or for checking if treatment was successful.
Endoscopy (EGD)
This is the most definitive way to diagnose an ulcer and is often recommended, especially if your symptoms are severe, you’re over 60, or if H. pylori tests are negative.
- What it Is: A thin, flexible tube with a camera on the end is passed down your throat, through your esophagus, stomach, and into the duodenum.
- What it Sees: The doctor can directly visualize the lining, identify ulcers, and check for bleeding.
- Biopsy: During the endoscopy, small tissue samples (biopsies) can be taken to test for H. pylori or to rule out other conditions like cancer.
Barium Swallow (Upper GI Series)
Less common now due to the widespread use of endoscopy, but still an option. You drink a liquid containing barium, which coats your digestive tract, making ulcers visible on X-rays. It’s not as accurate as endoscopy and doesn’t allow for biopsies.
Stomach ulcers, also known as peptic ulcers, can be a painful condition that affects many individuals. Understanding the underlying causes and exploring various treatment options is essential for effective management. For those interested in a holistic approach to health, you might find it beneficial to read about sustainable practices that can contribute to overall well-being. Check out this insightful article on sustainable agriculture, which discusses how cultivating a greener future can positively impact our health and the environment.
Treating Ulcers: Getting You Back to Normal
| Metrics | Value |
|---|---|
| Prevalence | 10% of the population |
| Symptoms | Abdominal pain, bloating, nausea |
| Treatment | Antibiotics, acid-reducing medications |
| Complications | Bleeding, perforation, obstruction |
Good news! Most ulcers are treatable, especially once the underlying cause is identified. Treatment typically focuses on eradicating H. pylori (if present), reducing stomach acid, and protecting the stomach lining.
Eradicating H. pylori
If H. pylori is the culprit, treatment usually involves a combination of medications for 7 to 14 days, often called “triple therapy” or “quadruple therapy.”
- Antibiotics: Usually two different antibiotics (e.g., amoxicillin, clarithromycin, metronidazole, tetracycline) are prescribed to kill the bacteria.
- Proton Pump Inhibitor (PPI): A strong acid-reducing medication (e.g., omeprazole, lansoprazole, esomeprazole) to allow the ulcer to heal.
- Sometimes Bismuth Subsalicylate: (like Pepto-Bismol) can be added, as it helps protect the stomach lining and has some antibacterial properties.
It’s crucial to complete the entire course of antibiotics, even if you feel better, to ensure the infection is fully cleared and to prevent antibiotic resistance. Your doctor will likely re-test for H. pylori a few weeks after treatment to confirm eradication.
Reducing Stomach Acid
Whether H. pylori is present or not, controlling stomach acid is key to healing an ulcer.
- Proton Pump Inhibitors (PPIs): These are very effective. They work by blocking the “pumps” in your stomach that produce acid. Examples include omeprazole, esomeprazole, lansoprazole, pantoprazole, and rabeprazole. They are usually taken for several weeks to allow the ulcer to heal.
- H2-Blockers (Histamine Blockers): These medications reduce acid production by blocking histamine receptors in the stomach. Examples include famotidine (Pepcid) and cimetidine (Tagamet). They are generally less potent than PPIs but can still be effective for milder cases or as a follow-up.
- Antacids: These are over-the-counter medications that provide quick, temporary relief by neutralizing existing stomach acid. They don’t heal the ulcer but can help manage symptoms. They’re often used in conjunction with other treatments.
Protecting the Stomach Lining
- Sucralfate (Carafate): This medication forms a protective barrier over the ulcer, shielding it from acid and allowing it to heal. It needs to be taken on an empty stomach.
- Misoprostol (Cytotec): This medication is a synthetic prostaglandin that helps protect the stomach lining. It’s sometimes used for people who must continue taking NSAIDs and are at high risk for ulcers, though it has side effects.
Lifestyle Adjustments and When to Seek Help
While not direct causes, certain lifestyle factors can hinder healing and worsen symptoms.
- Stop NSAIDs (if possible): If your ulcer is due to NSAIDs, your doctor will advise you to stop taking them or switch to a different pain reliever that’s safer for your stomach (like acetaminophen). If NSAIDs are essential, your doctor might prescribe a PPI alongside them.
- Quit Smoking: Smoking hinders ulcer healing and increases the risk of recurrence.
- Limit Alcohol: Alcohol irritates the stomach lining and increases acid production.
- Manage Stress: While not a direct cause, stress can exacerbate symptoms. Finding healthy ways to manage stress (e.g., exercise, mindfulness, hobbies) can be beneficial.
- Diet: While spicy food doesn’t cause ulcers, some people find that certain foods (spicy, acidic, fatty) trigger or worsen their symptoms. Pay attention to what bothers you and adjust accordingly. There’s no universal “ulcer diet,” but generally, eating smaller, more frequent meals and avoiding trigger foods can be helpful.
Ulcers are a common and often curable condition. If you’re experiencing persistent stomach pain, especially that burning sensation, don’t ignore it. A visit to your doctor can help you get a proper diagnosis and start on the path to feeling better. With the right treatment, most ulcers heal within a few weeks, allowing you to get back to enjoying life without that nagging stomach pain.